Living with eczema presents daily challenges that extend far beyond simple dry skin. For individuals, this chronic condition can affect sleep quality and daily comfort. Understanding the fundamental nature of the condition and the current medical strategies available empowers patients to take an active role in their care. A clear grasp of these concepts allows for better communication with healthcare providers and more effective long-term eczema treatment.
What Is Eczema?
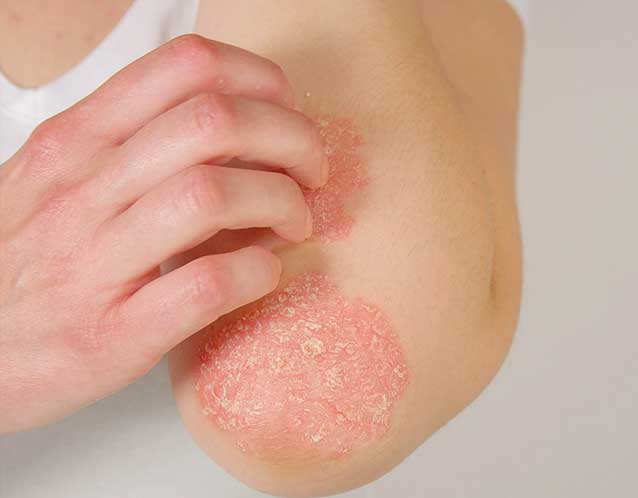
Eczema represents a group of conditions that cause the skin to become inflamed, irritated, and itchy. While it manifests differently in everyone, the core characteristic involves a compromised skin barrier. Healthy skin retains moisture and protects against outside elements, bacteria, and allergens. In those with eczema, the skin barrier does not function as efficiently. This dysfunction leads to moisture loss and allows irritants to enter, triggering an inflammatory response.
The symptoms vary in severity. Mild cases may present as patches of dry, slightly scaly skin. More severe instances involve intense itching, redness, cracking, and sometimes weeping sores. The condition is characterized by periods where symptoms flare up, followed by periods of remission. It is not contagious, meaning it cannot spread from person to person.
What Are the Causes and Types?
Pinpointing a single cause for eczema remains difficult because it typically results from a complex interplay of genetic and environmental factors. An overactive immune system also plays a central role. When the body encounters an irritant or allergen, the immune system reacts strongly, producing inflammation on the skin’s surface. While atopic dermatitis is the most common form, several other types exist. Contact dermatitis occurs when the skin touches an irritating substance. Dyshidrotic eczema causes small blisters on the hands and feet.
What Does Eczema Treatment Involve?
Modern dermatology focuses on a multi-pronged strategy to manage symptoms and prevent future flare-ups. No single cure exists yet, but current eczema treatment therapies offer significant relief. These include:
- Basic Skincare and Moisturizing: The foundation of all care plans involves maintaining the skin barrier. Regular application of moisturizers locks in water and improves the skin’s flexibility.
- Topical Therapies: For active inflammation, topical corticosteroids remain a standard prescription. These creams and ointments reduce swelling and redness swiftly.
- Systemic Medications and Biologics: For moderate to severe cases where topical treatments fail to provide relief, newer systemic options have changed the landscape of care. These engineered medications target specific parts of the immune system that drive inflammation.
- Phototherapy: Light therapy, or phototherapy, involves exposing the skin to ultraviolet (UV) light under medical supervision. This method helps reduce inflammation and can be highly effective for widespread eczema.
Seek Professional Dermatology Care
Managing a chronic skin condition requires a partnership with a qualified healthcare provider. While over-the-counter remedies provide temporary help for mild symptoms, a dermatologist offers the expertise needed to navigate the complexities of persistent eczema. They can accurately diagnose the specific type of dermatitis, identify potential triggers through testing, and prescribe advanced therapies like biologics or topical therapies if appropriate. Early intervention often prevents the condition from worsening and helps maintain a higher quality of life.
- Managing Vaginal Irritation and Tissue Sensitivity: Causes and Solutions
- Benefits of Regular Chiropractic Care for Improved Health and Mobility
- Understanding How Botox Works
- Understanding the Steps of Reconstructive Breast Surgery
- Understanding the Impact of Cognitive Behavioral Therapy on Mental Health