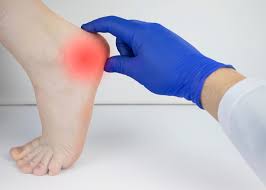
Heel pain can affect individuals of various ages and lifestyles; it often occurs at the bottom or back of the heel, making daily activities challenging. Everyday actions like walking, jogging, or standing for long periods sometimes trigger heel discomfort. Understanding what contributes to this issue and finding practical relief strategies is helpful for anyone looking to stay active and comfortable. Here are several frequent causes of heel pain and how to treat them:
Identifying Causes of Heel Pain
Several conditions or actions may trigger pain in your heel, including plantar fasciitis and Achilles tendinitis. Plantar fasciitis is a key cause of heel pain, and it affects the thick band of tissue running along the bottom of your foot. When this tissue gets inflamed, stabbing discomfort can occur with your first steps in the morning. Some people find that the pain fades with movement, only to return after standing too long or after getting up from sitting. The Achilles tendon connects the calf muscles to the heel bone, and overuse from exercise or repetitive strain sometimes leads to inflammation. People with Achilles tendinitis may notice pain and stiffness behind the heel, especially when they move more than usual.
Heel spurs are small, bony growths that form on the heel bone. While they sound serious, most heel spurs do not directly cause pain. Any discomfort often comes from inflamed tissue around the spur, which is commonly linked to conditions like plantar fasciitis. Stress fractures are another common cause of heel pain. Activities such as running or jumping create repetitive force on the heel. These actions may lead to tiny cracks called stress fractures, and unlike sudden injuries, the discomfort from a stress fracture tends to build up slowly. Recognizing the source of pain helps you take steps that are tailored and effective.
Approaching Heel Pain Relief Methods
People can apply various lifestyle adjustments and at-home strategies to help manage heel pain. The idea is to lower inflammation, protect the foot, and avoid actions that worsen discomfort. Several options include:
- Prioritizing Rest and Ice: Giving your feet a break is fundamental to recovery. Limit activities that place pressure on the heels, such as prolonged standing or running. Applying ice to the bottom of the foot, especially after activity, can help manage swelling and discomfort.
- Selecting Supportive Footwear: Footwear plays a key role in reducing heel pain. Focus on shoes with solid arch support and cushioned soles. Avoid walking barefoot, especially on hard surfaces, and contemplate replacing sneakers when they become too worn for proper support.
- Practicing Gentle Stretches: Gentle stretching is helpful, particularly for those dealing with plantar fasciitis or Achilles tendinitis. Stretching the calves, toes, and the bottoms of the feet may ease tightness. Try simple routines, such as calf stretches and towel stretches.
- Trying Heel Pads or Inserts: Heel pads, arch supports, or orthotic inserts provide extra cushioning. These devices help absorb shock, and they reduce the amount of stress placed on your heel. Over-the-counter options are usually accessible and can be a fundamental part of your comfort plan.
Visit a Foot and Ankle Specialist
Practical steps such as resting, wearing the right shoes, and practicing gentle stretches serve as key tools for relief. If these helpful strategies do not bring relief or if your pain intensifies, seek advice from a healthcare professional. A foot and ankle specialist can offer more targeted treatments, such as night splints or injection therapies. Contact an expert today to learn more about their foot and ankle services.